In the second time in as many years, the World Health Organization (WHO) has declared a new Global Public Health Emergency: the Zika virus crisis has been born. A new disease with another exotic name, Zika virus is predicted to infect millions in the next few months as it sweeps across the globe. Just as Ebola in West Africa is nearly out of the headlines – albeit still lingering on in Sierra Leone – the media has already pegged 2016 “the year of Zika”.
Like the Chinese lunar calendar, each year seems to have its own deadly, emerging pathogen. A recent commentary on Zika by the President of the American Society of Tropical Medicine & Hygiene asks us: “What’s next?” I’ll be honest and say that without a soothsayer, it is hard to pick from the over 500 other arthropod-borne viruses out there (not to mention other types of viruses, bacteria, fungi, prions and parasites) that are, unbeknownst to them, already competing for the 2017 title.
If I was a Victorian taxidermist, I would be envious of our modern “viral hunters” (disease biologists and ecologists). They have a vast unseen microbiological frontier open to discovery and cataloguing. The problem for the rest of us is that ‘discovery’ is only half the story; the messy world of global health and emerging diseases show that it isn’t quite like the laboratory bench.
Zoonoses
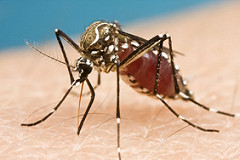
Like Ebola and the majority of other emerging diseases, Zika has an animal origin – in other words it a zoonoses. But while we might be forgiven our ignorance about Zika (first detected in 1947 along the shores of Lake Victoria in a rhesus monkey, it would be a faux pas not to know about its deadly vector, the aedes agypti mosquito .
The notoriety of this little arthropod started way before Zika, as it journeyed on shipping routes in the 1950s, and began breeding in the burgeoning urban cities of Asia and Latin America in old tires and household water jugs. From our own peri-domestic dwellings, it spread other arboviruses, such as Dengue fever, yellow fever and chikungunya. A recent study estimated that there are nearly 400 million dengue infections every year.
But the pandemonium around Zika has little to do with the majority of infections. Emerging on a series of Pacific Island States since 2007, Zika typically leads to mild febrile cases, with most being asymptomatic, that resemble dengue and chikungunya. In much of the tropics, inadequate diagnostic capacity and health services mean such illnesses are typically undiagnosed, unrecorded and forgotten about, even if some people do die. Among local communities there is often a widely repeated, but incorrect, maxim that “every fever is malaria”.
But with increasing cases of microcephaly in South America, Zika seems to be a different, more unpredictable beast. Certainly something to broadcast, understand and to act on… quickly
Crisis narrative
And that is exactly what is happening. The crisis narrative, the politics, the media, the uncertainty, the fear and the policy prescriptions and citizen reactions. Science and the biological intermixed with the social and political.
With the summer Olympics a matter of months away, troops have been deployed on the streets of Rio de Janeiro armed with fumigators, larvicide and information pamphlets – a new “war” against the mosquito has begun. The Health Minister of El Salvador, where gang violence has turned the country into one of the most violent places on earth, has been more draconian, and advised women in this deeply Catholic country to forgo pregnancy for the next two years while scientists figure out what is going on. Women’s rights activists have lashed out. Doesn’t the honorable Minister know that poor urban women in El Salvador are not the sole arbiters of when and how they get pregnant?
It’s a clear sign of desperation, of our limited understanding of how and why this unseen enemy has emerged. The US Centers for Disease Control and Prevention (CDC) have just reported a case of Zika being sexually transmitted in Texas.

We are told from the virologists that a vaccine is “at least” a decade away, if at all. Vector control will also be an uphill battle. Aedes agypti is incredibly resilient, and has often outsmarted conventional control techniques in the past, especially those that do not seek the involvement local communities. To add insult to injury, conspiracy theorists have begun crying foul, linking Zika emergence to a biotech experiment gone bad. Fears about GMOs have a new poster child.
The Zika virus has quickly become inseparable from a suite of other global challenges: unplanned urbanisation, poverty, women’s rights, social services for disabled newborns, climate change and dysfunctional political regimes. Entangled together, tensions mount and influence the different ways we respond.
One Health
While differences abound, we have been here before, many times. HIV/AIDS, Ebola, avian influenza, bovine spongiform encephalopathy (BSE), West Nile, Lyme disease, and the list goes on – albeit the characters and script are different. What past ‘lessons learnt’ have told us is that we need to take a new approach to these recurring pestilences: we should not be taken by surprise but plan for the inevitable. Paradoxically, that ‘inevitable’ is also uncertain and complex.
This is the central point of a huge body of post-Ebola literature that lays out clearly how we need to strengthen global surveillance, response and preparedness systems to better handle emerging diseases. We need a “One Health” approach that integrates human, animal and ecosystems health.
While this is all great and good, major disciplinary and socio-political divides remain that may bar our aspirations. Once the dust settles and the news cameras leave, as they have in West Africa, international pledges and lofty rhetoric to deal with the underlining ecological and social roots of these diseases tends to evaporate.
When social scientists talk about ‘political’ and ‘social’ dynamics we are not necessarily talking about exotic cultural practices. Power and politics are interwoven as much into the Vodou ritual dance as into the culture of global disease surveillance and response. This is becoming more and more accepted in public health circles, often under the rubric of ‘implementation science‘. I have shown previously on my research into rabies vaccination programmes, the control of pig-associated worm infections and zoonotic sleeping sickness, the importance of a social science approach in designing and implementing disease control interventions.
Global and local systems
Thinking about a more resilient and ultimately effective approach to emerging diseases requires asking difficult, sometimes uncomfortable, questions about current priorities and the structure of science and intervention. It demands delving into the complex relationships (and tensions) between global and local systems, policy and practice, science, technology and citizen participation, and different forms of knowledge and expertise.
This is the starting point for a new book I had the privilege of editing with colleagues from the Dynamic Drivers of Disease in Africa Consortium, entitled One Health: Science, politics and zoonotic disease in Africa. Over the book’s 11 chapters, we offer a much-needed political economy analysis of how zoonosis scientific research and policy networks are intertwined into systems of power, history, knowledge and politics. Ultimately, the book lays some groundwork for what we need on the journey ahead, and will be launched at One Health for the Real World, zoonoses, ecosystems and poverty, a symposium organised in collaboration with the Zoological Society of London.
But attention to social and political relationships is, again, only half the story. Social scientists themselves need to get out of their ivory tower. If the future is anything like the past, preventing and responding to future global health disasters will demand teamwork and self-reflection – the ability to work across multiple divides with creativity, political acumen and a dedication to social justice.
- Dr. Kevin Bardosh is a member of the Dynamic Drivers of Disease in Africa Consortium and a Research Scholar at the Division of Infection and Pathway Medicine, University of Edinburgh, and the Emerging Pathogens Institute, University of Florida. He currently runs an environmental health project in Haiti and is editor of the forthcoming book, One Health: Science, Politics and Zoonotic Disease in Africa to be published by Taylor and Francis in February 2016.
- An edited version of this blog was published on the BioMed Central ‘On Health’ blog.